1. Introduction
In modern healthcare systems, Electronic Health Records (EHR) and Clearinghouses are core components of the Revenue Cycle Management (RCM) pipeline. While EHR systems handle clinical and administrative data, clearinghouses act as intermediaries that validate, standardize, and transmit claims to insurance payers.
A healthcare clearinghouse is essentially a data transformation and routing engine that converts non-standard healthcare data into standardized formats and forwards it to payers for reimbursement .
2. High-Level Architecture
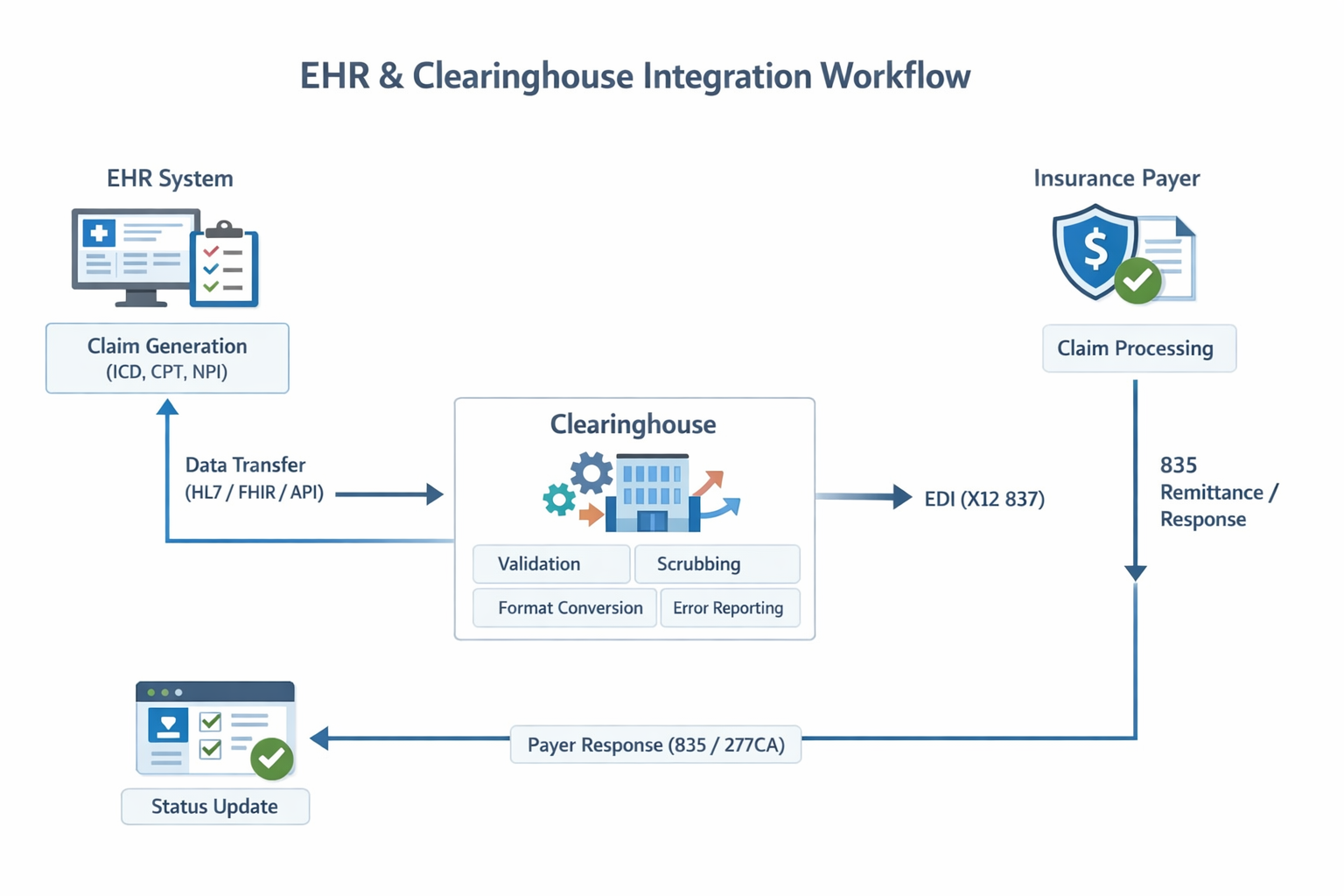
🔁 Integration Flow Overview
[EHR System]
↓
(Claim Generation)
↓
[Integration Layer / API / HL7/FHIR]
↓
[Clearinghouse]
↓
(Validation + Scrubbing + Transformation)
↓
[Insurance Payer]
↓
(Remittance Response)
↓
[Clearinghouse]
↓
[EHR System]
3. Core Components Involved
3.1 EHR System
- Stores patient data (demographics, diagnosis, procedures)
- Generates claims using:
- ICD-10 codes
- CPT codes
- Provider/NPI details
3.2 Clearinghouse
- Acts as middleware between provider and payer
- Responsibilities:
- Data normalization
- Claim validation (scrubbing)
- Format conversion (e.g., ANSI X12 837)
- Secure transmission
- Error reporting
Clearinghouses reduce claim errors and accelerate reimbursement cycles by validating and standardizing data before submission .
3.3 Payer (Insurance)
- Processes claims
- Sends responses (835 ERA, rejection reports)
4. Technical Integration Methods
4.1 HL7-Based Integration
HL7 International defines messaging standards for healthcare interoperability.
How it works:
- EHR sends data using HL7 messages (e.g., ORM, ORU)
- Middleware maps HL7 → EDI (X12 format)
- Clearinghouse processes it
-> HL7 enables different healthcare systems to communicate and exchange structured data consistently .
Example HL7 Flow:
MSH|^~\&|EHR|Hospital|Clearinghouse|...
PID|... (Patient Info)
FT1|... (Financial Transaction)
4.2 FHIR API-Based Integration (Modern Approach)
FHIR is a REST-based standard.
Features:
- JSON/XML APIs
- Real-time communication
- Easier than HL7 v2/v3
Example API Flow:
POST /Claim
{
"resourceType": "Claim",
"patient": {...},
"diagnosis": [...],
"procedure": [...]
}
FHIR uses modern web technologies (REST + JSON/XML) to exchange healthcare data efficiently .
4.3 Direct API Integration with Clearinghouse
Most clearinghouses provide:
- REST APIs
- SOAP APIs
- SFTP batch upload
Example:
POST /claims
Headers:
Authorization: Bearer API_KEYBody:
{
"claimData": {...}
}
5. Data Standards Used
| Standard | Purpose |
|---|---|
| ANSI X12 837 | Claim submission |
| ANSI X12 835 | Payment/remittance |
| HL7 v2/v3 | Clinical + admin messaging |
| FHIR | Modern API-based exchange |
| CDA | Clinical document exchange |
-> EDI claims (837) can contain hundreds of structured data elements, making mapping complex .
6. Step-by-Step Integration Workflow
Step 1: Claim Creation (EHR)
- Doctor completes encounter
- EHR generates claim data
Step 2: Data Mapping
- Internal format → Standard format
- Example: EHR Field → X12 Segment
patient_name → NM1
diagnosis → HI
Step 3: Transmission to Clearinghouse
- Via HL7 / FHIR / API
Step 4: Claim Scrubbing (Clearinghouse)
- Checks:
- Missing fields
- Invalid codes
- Insurance eligibility
Step 5: Format Conversion
- Non-standard → ANSI X12 837
Step 6: Submission to Payer
- Routing logic based on payer ID
Step 7: Response Handling
- 999 / 277CA (acknowledgements)
- 835 (payment)
Step 8: Back to EHR
- Status updated in EHR dashboard
7. Technical Architecture Patterns
7.1 Middleware-Based Integration
EHR → Integration Engine (Mirth / Kafka / Node.js) → Clearinghouse
Benefits:
- Loose coupling
- Scalability
- Retry logic
7.2 Event-Driven Architecture (Advanced)
EHR → Event Bus (Kafka)
→ Claim Processor Microservice
→ Clearinghouse API
Benefits:
- High throughput
- Real-time processing
- Fault tolerance
7.3 Microservices Approach
- Claim Service
- Eligibility Service
- Billing Service
- Clearinghouse Adapter Service
8. Security & Compliance
Required Standards:
- HIPAA compliance
- TLS encryption
- PHI protection
Security Layers:
- API authentication (OAuth2 / JWT)
- Data encryption (AES-256)
- Audit logs
Clearinghouses ensure secure transmission of protected health information (PHI) between providers and payers .
9. Common Challenges
9.1 Data Mapping Complexity
- EHR schema ≠ EDI schema
- Requires transformation engine
9.2 Interoperability Issues
- Different vendors
- Different standards
9.3 Claim Rejections
- Missing/incorrect codes
- Invalid patient data
9.4 Latency & Retry Handling
- Network failures
- API timeouts
10. Best Practices
Use Integration Engine
- Example: Mirth Connect
Implement Validation Layer Before Clearinghouse
- Reduce rejections
Use FHIR for New Systems
- Easier integration
Maintain Mapping Templates
- Version control for EDI mapping
Logging & Monitoring
- Track:
- Claim status
- Failures
- Response times
11. Real-World Example (Simplified)
Doctor enters diagnosis in EHR
→ EHR generates claim
→ Sends via API to clearinghouse
→ Clearinghouse validates + converts to 837
→ Sends to insurance
→ Insurance processes claim
→ Sends 835 response
→ Clearinghouse returns response to EHR
→ EHR updates billing dashboard
12. Conclusion
Integrating a clearinghouse with an EHR is a critical backend workflow in healthcare SaaS platforms. It involves:
- Data standardization (HL7, FHIR, X12)
- Middleware orchestration
- Secure communication
- Real-time or batch processing
A well-designed integration:
- Reduces claim rejection rates
- Improves cash flow
- Automates billing workflows
